Is my scar a keloid, or something else?
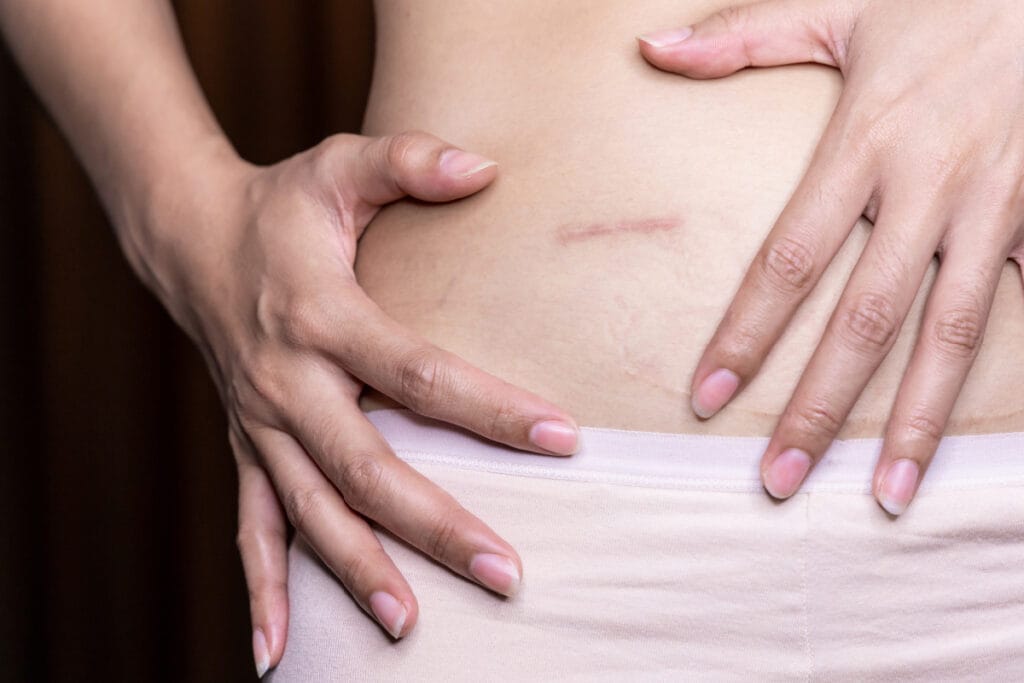
Your tummy tuck incision has healed, but the scar looks nothing like you expected. It’s thick, raised, and honestly concerning. Is it a keloid? A hypertrophic scar? Something else entirely?
These are important questions, as the type of scar you have determines how we approach treatment. Here are the characteristics that help us tell them apart.
What Makes Keloids Different
The defining characteristic of a keloid is that it grows beyond the boundaries of the original incision. If you had a facelift incision along your ear that’s now a raised scar extending onto your cheek or neck—skin that was never cut—you’re likely looking at a keloid.
Keloids don’t follow the normal rules of healing. Most surgical scars go through a predictable process: they’re red and slightly raised at first, then gradually flatten and fade over 12-18 months as they mature.
Keloids don’t do this. They keep producing collagen well past the point where healing should have stopped, and they can continue growing for months or even years after your procedure.
I’ve seen keloids develop from the smallest surgical incisions—an eyelid surgery (blepharoplasty) incision in the eyelid crease, a small excision site, even the tiny entry points from liposuction cannulas. The body’s response is completely disproportionate to the original incision. And once a keloid starts forming, it rarely goes away on its own.
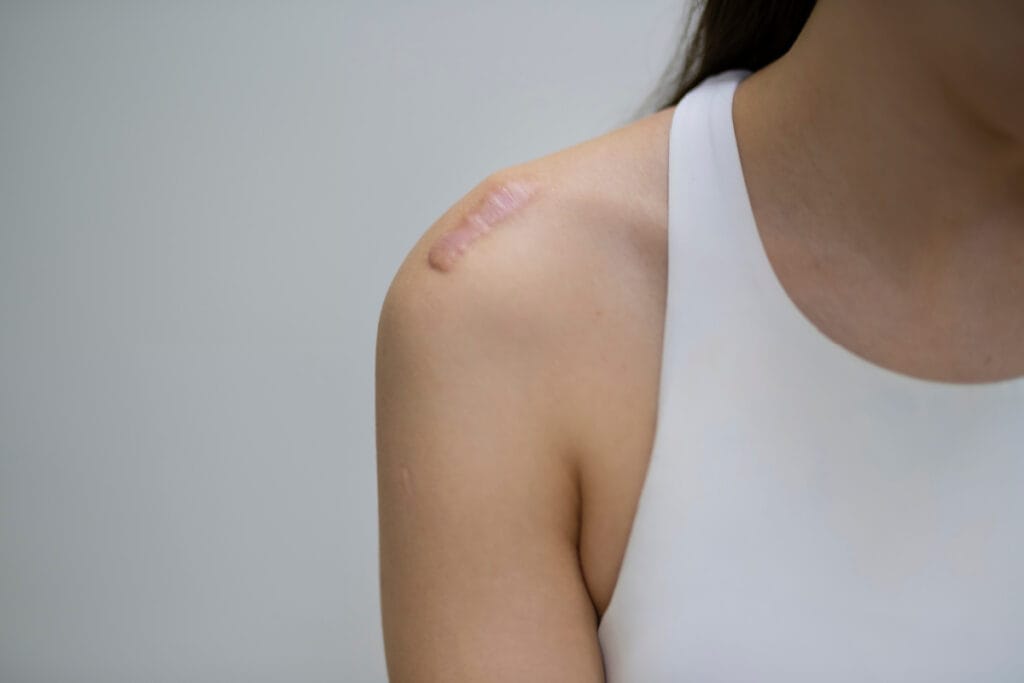
The appearance is distinctive too. Keloids often have a shiny, smooth surface with a firm or rubbery texture when you touch them. They can be darker than your surrounding skin and sometimes take on an irregular, almost tumor-like shape. Some patients describe them as looking like stretched, glossy skin pulled too tight over a bump.
Location matters quite a bit for cosmetic surgery scars. The chest and shoulders are particularly prone to keloid formation, which is something I discuss carefully with patients considering breast augmentation or reduction. Upper back procedures and any surgery near the earlobes also carry higher risk. These areas seem to trigger excessive collagen production more readily than others, which is why surgical technique and the closure method used matter so much in these locations.
Hypertrophic Scars: The More Common Reality
Contained Within the Incision
Here’s what I see far more often in my practice: hypertrophic scars after surgery. These are raised, thick scars that stay within the borders of the original incision. They can look quite dramatic and concerning to patients, but they behave very differently from keloids.
The key difference is containment. A hypertrophic scar from a tummy tuck incision might be raised and red and uncomfortable, but if you look closely, you’ll see it hasn’t spread beyond where the incision was made. It’s confined to exactly where tissue was cut.
Hypertrophic scars also tend to improve with time, even without treatment. I tell patients this might take a year or sometimes longer, but unlike keloids, these scars usually get the message to stop overproducing collagen and begin to soften and flatten.
Timing
Timing is another clue. Hypertrophic scars typically develop within the first few months after surgery. Keloids can show up much later—sometimes six months to a year after your incisions have seemingly healed.
The Role of Tension
Tension plays a significant role in hypertrophic scar formation after cosmetic surgery. Areas where skin is pulled or stretched during healing—tummy tuck incisions across the lower abdomen, breast lift incisions, body lift scars, anywhere the wound edges are under constant tension—are more likely to develop hypertrophic scars. This is why I’m so particular about surgical technique and incision placement. Reducing tension on healing tissue from the start, using layered closure techniques, and placing incisions strategically can prevent these scars from forming in the first place.
Who Develops Abnormal Scars
Genetic Predisposition
Genetics are powerful here. If your parents or siblings form keloids, your risk increases substantially. This isn’t just a casual family tendency—keloid formation appears to have a strong hereditary component, and knowing your family history helps me predict your risk before any cosmetic surgery procedure.
Skin Type and Ethnicity
Skin type matters tremendously. Keloids occur much more frequently in individuals with darker skin tones. Studies show significantly higher rates in people of African, Hispanic, and Asian descent compared to those with lighter skin. This doesn’t mean lighter-skinned individuals can’t develop keloids, but the risk is considerably lower.
Age Factors
Age is a factor I always consider. Younger patients, particularly those between 10 and 30 years old, have a higher rate of abnormal scarring. We think this relates to increased collagen production and faster cell turnover during these years.
What About Other Scars?
While keloids and hypertrophic scars account for most of the problematic scarring I treat, there are other types worth mentioning.
Atrophic scars sit below the skin surface rather than above it. These are the depressed scars you see after severe acne or chickenpox. The tissue loss creates small pits or indentations rather than raised tissue.
Contracture scars typically develop after burns and can actually restrict movement, particularly when they form over joints. The skin tightens and pulls, sometimes significantly limiting range of motion.
Occasionally, what appears to be a keloid turns out to be something more serious. I’ve had patients come in concerned about a “keloid” that was actually a dermatofibroma or, in rare cases, a type of skin cancer. This is why having an experienced physician evaluate any unusual scar growth is important.
How We Approach Treatment
Treatment strategy depends entirely on accurate diagnosis, which is why I examine scars carefully before recommending any intervention.
Options for Hypertrophic Scars
For hypertrophic scars, patience often pays off. Many of these scars improve substantially over time without any treatment. However, several approaches can accelerate improvement:
Treating Keloids Requires a Different Strategy
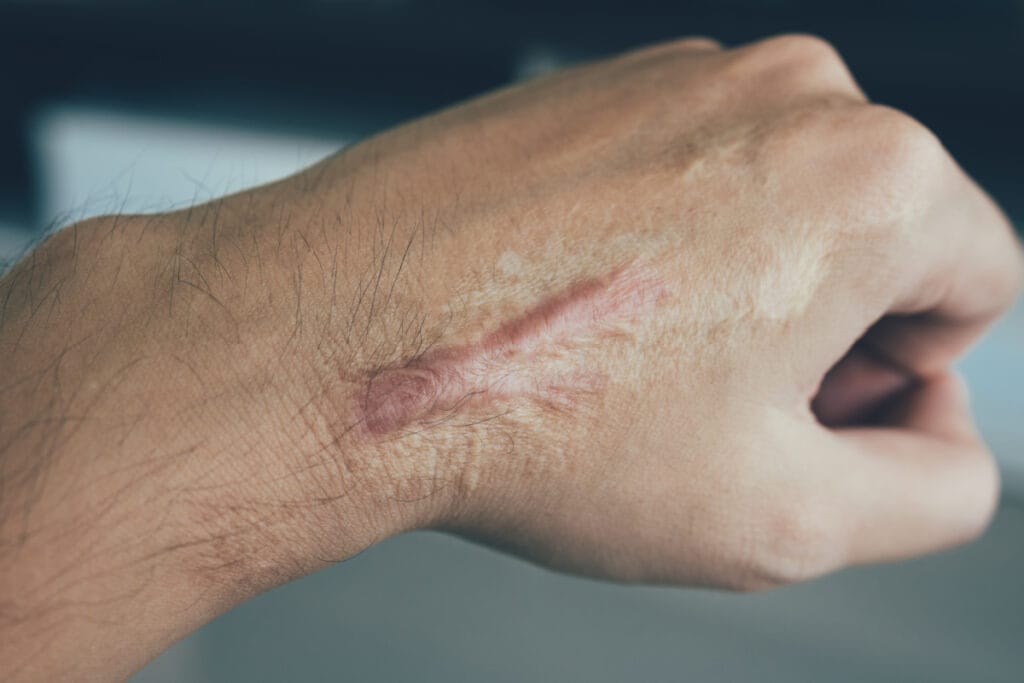
Keloids require a more aggressive, multi-modal approach because they’re notoriously resistant to single treatments. Surgical excision alone rarely works—keloids tend to grow back, often larger than before. When I do remove keloids surgically, I always combine the procedure with additional treatments like steroid injections or, in select cases, radiation therapy to prevent recurrence.
Cryotherapy uses extreme cold to reduce keloid size, and while it can be effective, results vary significantly from patient to patient.
In my experience, combining treatments typically produces better outcomes than relying on any single approach. The right combination depends on the scar’s location, size, symptoms, and how long it’s been present.
Prevention Strategies
If you know you’re prone to keloid formation, this becomes an important part of our surgical planning conversation. I need to know about any previous keloids or problematic scarring you’ve experienced, as this significantly influences which procedures might be appropriate and how I approach incision placement and closure.
Surgical Technique
Proper surgical technique matters immensely. When I perform surgery, meticulous closure technique—placing incisions in areas of minimal tension, using fine sutures, creating layered closures, avoiding excess tightness—makes a real difference in how scars heal. For patients at higher risk, I’m even more particular about these details.
Post-Operative Care
Following recovery instructions carefully, keeping incisions protected from UV exposure (which can darken scars), avoiding activities that put tension on healing incisions, and using any recommended scar care products all contribute to better healing.
Choosing the Right Sunscreen for Healing Scars
Sun protection on a healing scar isn’t optional. Ultraviolet exposure on immature scar tissue can cause permanent darkening (hyperpigmentation) that’s extremely difficult to reverse, so which sunscreen you choose actually matters.
The two main categories—physical (also called mineral) and chemical sunscreens—work in fundamentally different ways.
Early Intervention
If you notice a surgical scar becoming unusually thick or spreading beyond the incision line, contacting me sooner rather than later often leads to better outcomes.
When to Seek Evaluation
You should contact me about a surgical scar if it’s growing beyond the original incision line, continuing to expand months after your procedure, causing significant pain or itching, restricting your movement (particularly with body contouring scars), or simply bothering you cosmetically.
Accurate diagnosis makes all the difference. While you can find plenty of scar images online, nothing replaces an in-person examination where I can assess the scar’s texture, review your surgical history and healing process, and discuss treatment options specific to your situation.
At my Bellevue cosmetic surgery practice, I personally evaluate every patient with problematic scarring. We can discuss whether you’re dealing with a keloid, hypertrophic scar, or something else entirely, and develop a treatment approach that makes sense for your specific circumstances.
Give us a call at (425) 453-9060 or contact us online to schedule your complimentary consultation.
References »
Limandjaja, G. C., Niessen, F. B., Scheper, R. J., & Gibbs, S. (2020). Hypertrophic scars and keloids: Overview of the evidence and practical guide for differentiating between these abnormal scars. Experimental Dermatology, 29(1), 110-126. https://doi.org/10.1111/exd.14121
McGinty, S., & Siddiqui, W. (2023). Keloids. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK507899/
Ogawa, R. (2017). Keloid and hypertrophic scars are the result of chronic inflammation in the reticular dermis. International Journal of Molecular Sciences, 18(3), 606. https://doi.org/10.3390/ijms18030606
Berman, B., Maderal, A., & Raphael, B. (2017). Keloids and hypertrophic scars: Pathophysiology, classification, and treatment. Dermatologic Surgery, 43(Suppl 1), S3-S18. https://doi.org/10.1097/DSS.0000000000000819
Ud-Din, S., & Bayat, A. (2016). Non-surgical management of keloid disease. BMJ, 353, i2992. https://doi.org/10.1136/bmj.i2992
Mustoe, T. A. (2008). Evolution of silicone therapy and mechanism of action in scar management. Aesthetic Plastic Surgery, 32(1), 82–92. https://doi.org/10.1007/s00266-007-9030-9
O’Brien, L., & Jones, D. J. (2013). Silicone gel sheeting for preventing and treating hypertrophic and keloid scars. Cochrane Database of Systematic Reviews, (9), CD003826. https://doi.org/10.1002/14651858.CD003826.pub3
Puri, N., & Talwar, A. (2009). The efficacy of silicone gel for the treatment of hypertrophic scars and keloids. Journal of Cutaneous and Aesthetic Surgery, 2(2), 104–106. https://doi.org/10.4103/0974-2077.58527
Gold, M. H., McGuire, M., Mustoe, T. A., Pusic, A., Sachdev, M., Waibel, J., & Murcia, C. (2014). Updated international clinical recommendations on scar management: Part 2—Algorithms for scar prevention and treatment. Dermatologic Surgery, 40(8), 825–831. https://doi.org/10.1111/dsu.0000000000000050
Fitzpatrick, R. E. (1999). Treatment of inflamed hypertrophic scars using intralesional 5-FU. Dermatologic Surgery, 25(3), 224–232. https://doi.org/10.1046/j.1524-4725.1999.08165.x
Haurani, M. J., Foreman, K., Yang, J. J., & Siddiqui, A. (2009). 5-Fluorouracil treatment of problematic scars. Plastic and Reconstructive Surgery, 123(1), 139–148. https://doi.org/10.1097/PRS.0b013e3181904d1b
Nanda, S., & Reddy, B. S. (2004). Intralesional 5-fluorouracil as a treatment modality of keloids. Dermatologic Surgery, 30(1), 54–57. https://doi.org/10.1111/j.1524-4725.2004.30005.x
Shah, V. V., Aldahan, A. S., Mlacker, S., Alsaidan, M., Samarkandy, S., & Nouri, K. (2016). 5-Fluorouracil in the treatment of keloids and hypertrophic scars: A comprehensive review of the literature. Dermatology and Therapy, 6(2), 169–183. https://doi.org/10.1007/s13555-016-0118-5
Hanson, K. M., Gratton, E., & Bardeen, C. J. (2006). Sunscreen enhancement of UV-induced reactive oxygen species in the skin. Free Radical Biology and Medicine, 41(8), 1205–1212. https://doi.org/10.1016/j.freeradbiomed.2006.06.011
Matta, M. K., Florian, J., Zusterzeel, R., et al. (2020). Effect of sunscreen application on plasma concentration of sunscreen active ingredients: A randomized clinical trial. JAMA, 323(3), 256–267. https://doi.org/10.1001/jama.2019.20747
Due, E., Rossen, K., Sorensen, L. T., Kliem, A., Karlsmark, T., & Haedersdal, M. (2007). Effect of UV irradiation on cutaneous cicatrices: A randomized, controlled trial with clinical, skin reflectance, histological, immunohistochemical and biochemical evaluations. Acta Dermato-Venereologica, 87(1), 27–32. https://doi.org/10.2340/00015555-0154
Sander, M., Sander, M., Burbidge, T., & Beecker, J. (2020). The efficacy and safety of sunscreen use for the prevention of skin cancer. CMAJ, 192(50), E1802–E1808. https://doi.org/10.1503/cmaj.201085
U.S. Food and Drug Administration. (2021). Sunscreen: How to help protect your skin from the sun. https://www.fda.gov/drugs/understanding-over-counter-medicines/sunscreen-how-help-protect-your-skin-sun
Darougheh, A., Asilian, A., & Shariati, F. (2009). Intralesional triamcinolone alone or in combination with 5-fluorouracil for the treatment of keloid and hypertrophic scars. Clinical and Experimental Dermatology, 34(2), 219–223. https://doi.org/10.1111/j.1365-2230.2007.02631.x
Khalid, F. A., Mehrose, M. Y., Saleem, M., Yousaf, M. A., Mujahid, A. M., Rehman, S. U., Ahmad, S., & Tarar, M. N. (2019). Comparison of efficacy and safety of intralesional triamcinolone and combination of triamcinolone with 5-fluorouracil in the treatment of keloids and hypertrophic scars. Burns, 45(1), 69–75. https://doi.org/10.1016/j.burns.2018.08.011
Ren, Y., Zhou, X., Wei, Z., Lin, W., Fan, B., & Feng, S. (2017). Efficacy and safety of triamcinolone acetonide alone and in combination with 5-fluorouracil for treating hypertrophic scars and keloids: A systematic review and meta-analysis. International Wound Journal, 14(3), 480–487. https://doi.org/10.1111/iwj.12629
Davison, S. P., Dayan, J. H., Clemens, M. W., Sonni, S., Wang, A., & Crane, A. (2009). Efficacy of intralesional 5-fluorouracil and triamcinolone in the treatment of keloids. Aesthetic Surgery Journal, 29(1), 40–46. https://doi.org/10.1016/j.asj.2008.11.006